Beta Brain Waves:
The Complete Science Guide
What they are, how they work, what happens when they're out of balance — and what the latest neuroscience research from MIT, Brown University, and Stanford actually says about them.
01What Are Beta Brain Waves?
Your brain never stops generating electricity. Right now, as you read these words, approximately 86 billion neurons are firing electrochemical signals at varying speeds, and when large populations of them synchronize, they create measurable rhythmic patterns — oscillations we call brain waves. Electroencephalography, or EEG, has allowed scientists to detect and record these patterns since the 1920s, and over a century of research has mapped them into distinct frequency bands, each associated with different mental states and functions.
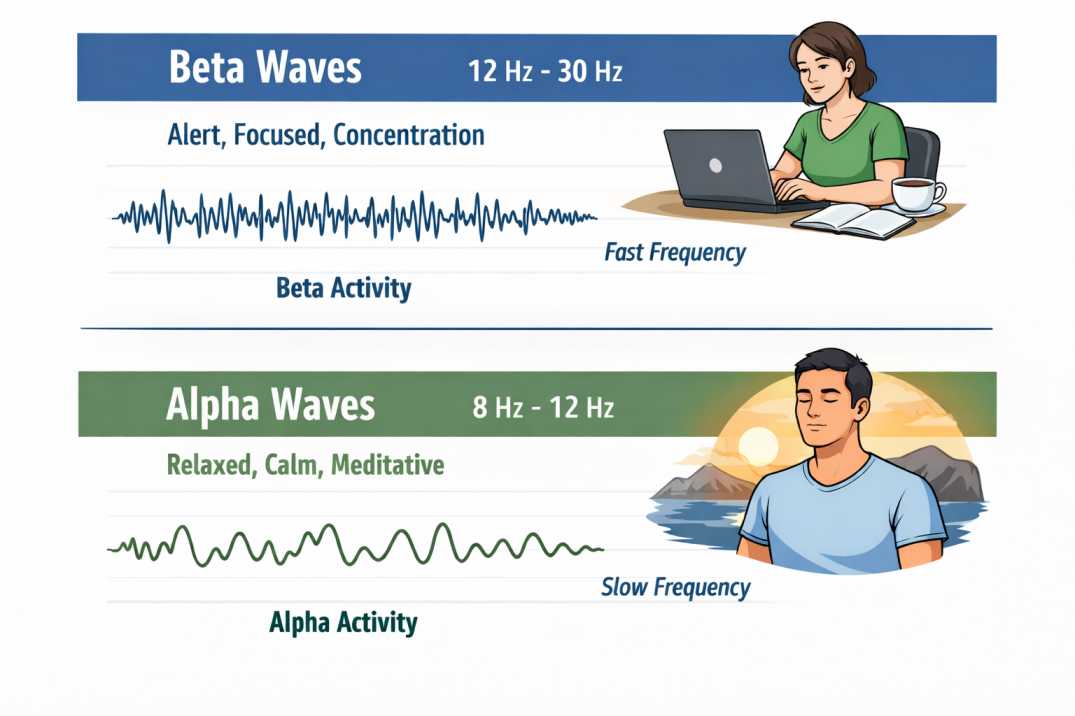
Beta brain waves occupy the 12 to 30 Hz range — meaning they cycle between 12 and 30 times per second. They are the dominant frequency when you are actively awake, thinking, processing information, having a conversation, or solving a problem. If you are reading this article with conscious attention, beta waves are almost certainly playing a central role in your brain's activity right now.
The critical thing to understand from the outset: beta waves are not inherently good or bad. They exist on a spectrum. Too little, and you can't concentrate, can't engage, can't execute — your brain is underperforming for the task at hand. Too much, especially in the high-frequency range, and you're anxious, exhausted, overwhelmed, and unable to settle. The goal is always appropriate beta activity for the context — and that standard changes throughout the day and across different tasks.
02The Full Brainwave Spectrum — Where Beta Fits
To understand beta waves properly, you need to see where they sit within the broader architecture of brain activity. The EEG frequency spectrum runs from the very slow (under 1 Hz in deep unconscious states) to the very fast (above 80 Hz in some gamma research). For practical purposes, five main bands are studied clinically and scientifically:
0.5–4 Hz
4–8 Hz
8–12 Hz
12–15 Hz
15–20 Hz
20–30 Hz
30–100 Hz
An important correction to popular neuroscience content: no single brainwave is "the good one." Healthy cognition depends entirely on flexibility — the brain's ability to move fluidly between appropriate states as context demands. A brain stuck in high beta all day is not performing well. Neither is one that can never produce enough beta to sustain focus. The measure of a healthy brain is not which waves dominate, but how smoothly and appropriately it transitions between them.
03The 3 Beta Sub-bands — Explained in Plain Language
Not all beta activity is the same. The scientific literature consistently distinguishes three sub-bands within the 12–30 Hz range, each with distinctly different cognitive and physiological associations. Understanding this distinction is critical — because much of what people misunderstand about beta waves comes from treating it as a single, uniform state.
When people say "beta waves cause anxiety," they almost always mean high beta (20–30 Hz) in excess. When people say "I need more focus and less brain fog," they usually need more low beta / SMR (12–15 Hz). These are different problems requiring different solutions — and conflating them is the source of most confusion in popular brainwave content.
04What MIT Research Actually Says About Beta Waves
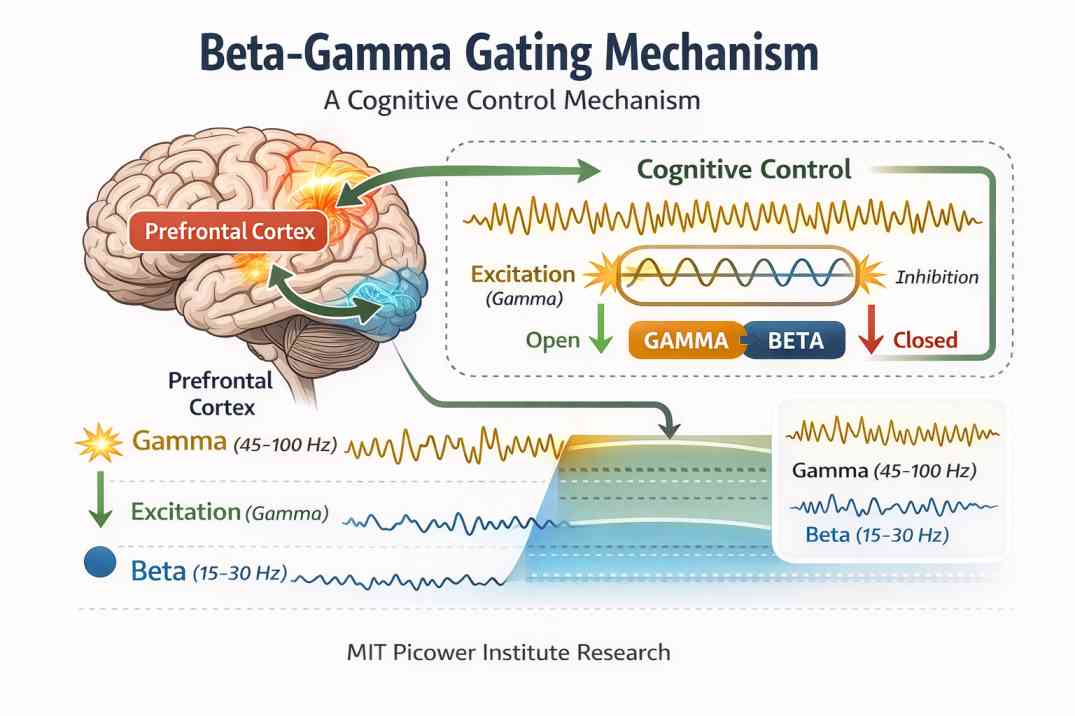
The most significant recent advance in beta wave research came from MIT's Picower Institute, where neuroscientist Earl Miller and his team conducted a series of landmark studies on how beta rhythms function as a cognitive control mechanism. This research fundamentally changed how the neuroscience community understands what beta waves actually do — and the answer is far more sophisticated than "they help you focus."
Miller's team found that beta waves function as a gating mechanism for working memory. They regulate which pieces of information are allowed to enter and exit your active mental workspace at any given moment. When beta waves rise, they suppress gamma waves — and gamma is associated with encoding new sensory information. This means beta is literally the brain's way of saying "hold on, keep processing what we already have — don't let new input in yet."
The practical implication is significant: beta bursts are how your brain maintains mental goals under pressure. Each burst reinforces the current cognitive task, keeping it stable against distraction. Without adequate beta activity, goals and intentions literally become unstable in the brain — which is precisely what happens in certain subtypes of ADHD and other attention disorders.
Separately, researchers at Brown University proposed a new biophysical theory of how beta waves arise in the brain — establishing that they originate largely in the thalamus and travel to specific cortical locations, occurring in quick but powerful bursts lasting at most 150 milliseconds. This transient nature is important: beta is not a sustained hum but a series of discrete gating events, each one briefly reinforcing a cognitive state before releasing it. Understanding this changes how clinicians and researchers think about modulating beta — you're not trying to raise a background level, you're trying to influence the frequency and strength of these bursts.
05Too Much vs Too Little — What the Research Shows
The research is unambiguous on both ends of the spectrum. Here is a precise, evidence-grounded breakdown of what excessive and insufficient beta activity looks like in clinical and everyday contexts:
- Chronic anxiety, generalised worry, and hypervigilance
- Insomnia — inability to downshift from active thinking at bedtime
- OCD tendencies and repetitive, intrusive thought loops
- Irritability, agitation, and emotional reactivity
- Racing mind — difficulty sustaining any single thought chain
- Gastrointestinal distress, muscle tension, elevated heart rate
- Mental exhaustion despite apparent wakefulness
- Bipolar tendencies in some clinical presentations (per CAD-AZ)
- High beta should not exceed 10% at any brain site in resting state
- ADHD symptoms — difficulty initiating and sustaining attention
- Brain fog, mental sluggishness, inability to "get going"
- Poor academic and cognitive performance
- Depression — particularly low engagement and low motivation subtypes
- Daydreaming during tasks that require active concentration
- Difficulty with problem-solving and sequential thinking
- Reduced reading speed and comprehension
- Learning disabilities involving sequencing and calculation
- Deficiency of 13 Hz activity specifically impairs math and sequencing tasks
These associations are correlational and clinically observed — not simple cause-and-effect. A person experiencing anxiety does not necessarily have "too much" beta everywhere in their brain. EEG assessment requires trained clinicians to interpret site-specific and context-specific data. If you suspect a clinical brainwave imbalance, a quantitative EEG (qEEG) assessment by a qualified practitioner is the appropriate path — not self-diagnosis from frequency descriptions alone.
06Beta Waves, ADHD, and Anxiety — The Clinical Connection
Two conditions dominate the clinical conversation around beta wave imbalance: ADHD and anxiety disorders. They represent opposite ends of the beta spectrum, and understanding the distinction matters practically for anyone exploring this field.
Beta Waves and ADHD
In many individuals with ADHD, EEG measurements reveal a deficit of SMR and low beta activity (12–15 Hz), particularly in the sensorimotor cortex. The brain defaults to theta rhythms (4–8 Hz) — the frequency associated with daydreaming — when it should be generating alert, focused beta. This creates the characteristic pattern of cognitive engagement followed by rapid drift that defines ADHD inattention.
Neurofeedback's most established application is in ADHD treatment using beta enhancement protocols. Multiple peer-reviewed studies show that training participants to increase SMR and suppress theta activity produces measurable improvements in attention, impulse control, and academic performance. More than three out of four children with ADHD show significant improvement after neurofeedback training targeting these specific frequency ranges, according to clinical meta-analyses.
| Condition | Beta Pattern | Target Band | Intervention Direction |
|---|---|---|---|
| ADHD (Inattentive) | Low SMR / Low beta (12–15 Hz) | SMR 12–15 Hz | Increase SMR, suppress theta |
| Generalised Anxiety | Excess high beta (20–30 Hz) | High Beta 20–30 Hz | Reduce high beta, increase alpha |
| Depression (low-energy) | Low beta + excess alpha frontal | Mid Beta 15–20 Hz | Increase beta, reduce frontal alpha |
| Epilepsy (SMR protocol) | Irregular sensorimotor beta | SMR 12–15 Hz | Enhance SMR, reduces seizure frequency |
| Parkinson's Disease | Abnormal beta bursts in motor cortex | Motor Beta | Research ongoing — DBS targets |
Beta Waves and Anxiety
Anxiety and beta have a more complex relationship than most popular sources convey. Anxiety is not simply "too much beta everywhere." Research consistently shows that excess in the high-beta band (20–30 Hz) correlates with the subjective and physiological markers of anxiety — racing thoughts, physical tension, hypervigilance, and the inability to downregulate after stressors. A 2025 EEG study published in Biological Psychiatry confirmed distinct periodic and aperiodic beta signatures in individuals with major depressive disorder versus anxiety disorders, suggesting the patterns are clinically distinguishable, not interchangeable.
Crucially, people with anxiety often have sufficient or even excess beta overall, but the wrong distribution — too much high beta, not enough low beta or alpha as a counterbalance. The therapeutic goal is not to suppress beta entirely but to shift the balance toward the lower, calmer end of the frequency range while supporting alpha as a natural downregulator.
077 Evidence-Based Ways to Optimise Your Beta Activity
Before listing these methods, one honest clarification: you cannot target specific Hz frequencies with a general lifestyle change. What you can do is support conditions that encourage your brain to produce healthier, more balanced beta activity over time. Here is what the current evidence actually supports:
If your goal is to reduce excessive high beta (anxiety, racing thoughts), the most evidence-backed approaches are: regular aerobic exercise, meditation (which reliably increases alpha and reduces high beta), controlled breathing protocols, and neurofeedback with alpha/high-beta inhibition protocols. Addressing sleep quality is also critical — sleep deprivation consistently elevates high-beta activity during waking hours.
08Neurofeedback and Beta Training — What the Research Shows
Neurofeedback is the most direct, studied, and clinically established method for intentionally modifying beta wave patterns. It works through operant conditioning: sensors attached to the scalp continuously monitor your brainwave activity, and the system provides real-time feedback — typically visual or auditory — that rewards your brain when it produces the target frequency and withdraws the reward when it drifts away.
The brain, naturally seeking reward, learns to produce the rewarded frequency pattern more reliably over time. For beta training specifically, the most established protocols include:
| Protocol | Target | Clinical Application | Evidence Level |
|---|---|---|---|
| SMR Enhancement | Increase 12–15 Hz, suppress theta | ADHD, focus deficits, epilepsy, sleep | Level 4 — Strong |
| Beta Enhancement | Increase 15–18 Hz, suppress theta | ADHD hyperactive, cognition, reading | Level 4 — Strong |
| High Beta Inhibition | Reduce 20–30 Hz, increase alpha | Anxiety, OCD, stress, insomnia | Level 3 — Good |
| Alpha/Theta (cross-band) | Increase alpha/theta, inhibit beta | PTSD, trauma, addiction | Level 3 — Good |
SMR neurofeedback — training the sensorimotor rhythm at 12–15 Hz — has been studied for over 50 years and carries the strongest evidence base. A study on improving golf putting performance using SMR neurofeedback demonstrated enhanced focus and automaticity during skill execution — an effect that generalises to other performance contexts. Research on elderly adults shows SMR training can reverse cognitive decline and improve working memory, suggesting applications well beyond clinical ADHD treatment.
In the United States, neurofeedback is offered by licensed practitioners in most major cities and is used in both clinical and performance-enhancement contexts. In Europe, availability varies significantly by country. UK practitioners are typically registered with the British Psychological Society (BPS) or similar bodies. Germany, the Netherlands, and Scandinavia have established neurofeedback clinical networks. France and Southern European countries have fewer practitioners but growing interest. Home neurofeedback devices (Muse, NeuroSky, OpenBCI) are available across all regions as entry-level options, though they lack the precision of clinical EEG systems.
09Beta vs All Other Brainwaves — The Complete Comparison
Context is everything in brainwave science. Here is how beta compares to the other four major bands across the key variables that matter for practical understanding:
| Brainwave | Frequency | Primary State | Cognitive Role | Excess Sign |
|---|---|---|---|---|
| Delta | 0.5–4 Hz | Deep sleep, unconscious | Repair, immune, unconscious processing | Brain injury, extreme fatigue |
| Theta | 4–8 Hz | Daydream, hypnagogic | Creativity, memory, subconscious | ADHD drift, inattention |
| Alpha | 8–12 Hz | Relaxed, eyes closed | Idle mode, emotional regulation | Frontal: depression, ADD |
| Beta | 12–30 Hz | Alert, active, thinking | Focus, working memory gating, control | Anxiety, insomnia, OCD |
| Gamma | 30–100 Hz | Peak cognition, perception | Sensory binding, insight, integration | Rare; some seizure patterns |
The relationship between beta and alpha deserves particular attention. In a well-regulated brain, alpha and beta exist in a reciprocal, see-saw relationship. When beta rises, alpha typically decreases — and vice versa. This is why relaxation practices that increase alpha (meditation, slow breathing, yoga) also effectively reduce excess beta. And why sustained high beta tends to push alpha out of the picture, leaving the brain without its natural calm counterpart.
10Frequently Asked Questions
Beta Is Not Your Enemy — Imbalance Is
Beta brain waves are your brain's operating mode for conscious, engaged, goal-directed life. The neuroscience is clear: they gate working memory, sustain cognitive goals under pressure, and underpin every act of focused attention. The problem is never beta itself — it's too much of the wrong kind, or not enough of the right kind, at the wrong time. Understanding that distinction is the first step toward actually doing something about it.